Do you have access to healthy foods, transportation to a doctor, high-speed internet for telemed appointments, or a roof over your head? These are assumptions that most of us take for granted, and are not the questions that insurers usually take into consideration. But, as they look to increase member outcomes and foster long-term customer loyalty, considering the changing needs of many consumers in the face of today’s current affairs, it’s time they did.
In fact, forward-looking health plans
Read More
Medicare Advantage | Payers | News, Analysis, Insights
The New Normal: Rethinking Healthcare Delivery in a Post-COVID World
It’s becoming clearer that, while we are all hoping that things are going to go back to the way things were at the beginning of the year, the COVID-19 crisis will result in a new normal. That’s especially true in healthcare, due to four issues that are being wildly amplified by the COVID-19 crisis. Namely:
1. The US government has huge deficits, and healthcare is a major driver of the unsustainable increase in these deficits.
2. Addressing the demand for healthcare as a right (not a
Read More
Inovalon Launches FHIR-Based Solution for Health Plan Compliance
What You Should Know:
- Inovalon announced the availability of its Cloud-Based “Consumer Health Gateway” Module, alleviating the need for health plans to build their own Patient Access API to comply with the new requirement of the 21st Century Cures Act.
- The Consumer Health Gateway is a consumer portal allowing the FHIR®-based exchange of a patient’s claims and clinical data securely with authorized third-party applications. It consists of a robust patient consent and authentication
Read More
How AI-Driven Insight Could Fuel Medicare Advantage Success
Medicare Advantage plans need more than consumer-centric design, payer/provider alignment, and strong connections across the continuum of care to drive value. The high-value performance also depends on their ability to use data to make a meaningful difference in members’ health.
With 11,000 people aging into Medicare daily, proficiency in managing Medicare Advantage populations is critical for demonstrating value in a competitive market. Enrollment in these plans is growing significantly,
Read More
Aledade Raises $64M for Value-Based Care Network of Physician-Led ACOs
What You Should Know:
- Aledade raises $64M in Series C funding led by OMERS Growth Equity to expand its national network of more than 500 physician-driven accountable care organizations (ACOs) across 27 states.
- To date, Aledade’s ACOs care for more than 840,000 patients and manage more than $7.5 billion in health care spending through 38 Medicare and 42 other value-based contracts.
Today, Aledade announced
it has closed a $64 million Series C funding round following the
Read More
Addressing Loneliness and Social Isolation in the Medicare Population
In recent years, the healthcare industry's understanding of social determinants of health (SDoH) and their impact on patient outcomes has grown dramatically. Researchers and practitioners now recognize that social isolation and loneliness fall under the SDOH umbrella. In response, many payers and providers are exploring initiatives to address social isolation among members and patients.
The health effects of social isolation and loneliness are costly and harmful. According to Health
Read More
Puerto Rico’s First Home Delivery Pharmacy Launches During COVID-19 Crisis
What You Need to Know:
- Pharmacy benefits manager Abarca and Triple-S Salud announced the launch of Triple-S en Casa, Puerto Rico’s first prescription home delivery program during the COVID-19 crisis.
- Developed in partnership with one of the Island's largest health plans and pharmacy networks, Triple-S en Casa lets consumers manage and order their prescriptions through an easy-to-use mobile app--and have them delivered by a local pharmacy.
Pharmacy benefits manager Abarca and
Read More
Vivify Health Launches COVID-19 Screening, Self-Isolation and Monitoring Pathways
What You Need to Know:
- Vivify Health has announced that availability today of new COVID-19 Screening, Self-Isolation and Monitoring Pathways for Vivify+Go mobile solution to providers at non-cost.
- This enables low-risk patients or those with mild symptoms to use their mobile devices to self-screen for COVID-19 by answering a series of questions that follow the current Centers for Disease Control and Prevention (CDC) guidelines.
- The self-screening helps providers scale their
Read More
Benefits of Store and Forward, or Asynchronous Telehealth Solutions
An introduction to asynchronous, or store-and-forward, as a modality of telehealth
As our healthcare system continues to innovate in order to meet demands and improve the delivery of value, various telehealth solutions have emerged and been implemented to increase efficiency, access to, and quality of care. Telehealth is a broad term encompassing “a collection of technology-based means or methods to enhance healthcare delivery and education.” As defined by the National Telehealth
Read More
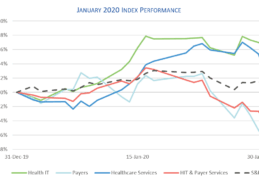
Analysis: January Health IT M&A Activity; Public Company Performance
– Healthcare Growth Partners’ (HGP) summary of Health IT/digital health mergers & acquisition (M&A) activity, and public company performance during the month of January 2020.
Ten years into the bull market, we operate in a heightened state of awareness for any indication of market weakness that may signal a downturn. While debt levels are rising and GDP growth somewhat sluggish, the world of private equity, public equity, and M&A continues to be in full swing bull market
Read More