What You Should Know:
– A new Accenture report called “Breakthrough Behavioral Health Access: Think Virtual” finds that the use of virtual behavioral health could expand care for more than 53 million Americans facing these conditions.
– Demand for behavioral health specialists significantly outweighs current availability; in addition to severe wait times of 25 days for first clinical appointments, we are projected to have a shortage of 250,000 behavioral health and mental health professionals by 2025.
– Just a 1% increase in treatment for these disorders would save $2.4 billion annually and could yield as much as $2.4 billion in medical cost savings annually.
The use of virtual delivery channels could expand treatment to 53 million Americans suffering from behavioral health issues, according to a new report from Accenture. The report, “Breakthrough Behavioral Health Access: Think Virtual,” is based on a survey of more than 3,400 people in the U.S. diagnosed with or having symptoms related to specific behavioral health conditions such as anxiety, depression, post-traumatic stress syndrome, attention deficit disorder or reported themselves as having addiction or substance abuse issues.
Access to Behavioral Healthcare Barriers
Access to behavioral healthcare is especially challenging. Beyond the burden on individuals, the challenges of accessing and delivering behavioral health services have a ripple effect across healthcare. Payers, providers, employers, government and life sciences companies are all impacted differently.
“The behavioral health crisis in the U.S. isn’t new, but the pandemic is clearly exacerbating it,” said Rich Birhanzel, a senior managing director at Accenture who leads the company’s Health practice globally. “The rapid expansion of virtual care models during lockdown in the current pandemic created new expectations for effective and reliable healthcare at a distance. While our research found that only 38% of respondents hadn’t been widely using a virtual channel for such treatment in the prior three years, they’re now overwhelmingly willing to do so.”
Virtual Health Can Shatters Barriers
Current data indicates that nearly 58 million adults and
8 million youth between the ages of six and 17 in the U.S. have mental
health and/or substance use disorders, yet only 43% of affected adults are receiving
treatment for them. Four in five respondents (81%) of the Accenture survey said
they would either definitely or probably engage in a virtual channel to manage
their behavioral health condition. Applying this finding to the 66 million
adults and youths impacted by these disorders suggests that virtual channels
could expand care to approximately 53 million people. Furthermore, the number
of people with such conditions is likely to rise due to the current environment
of COVID-19, record unemployment, and widespread social unrest.
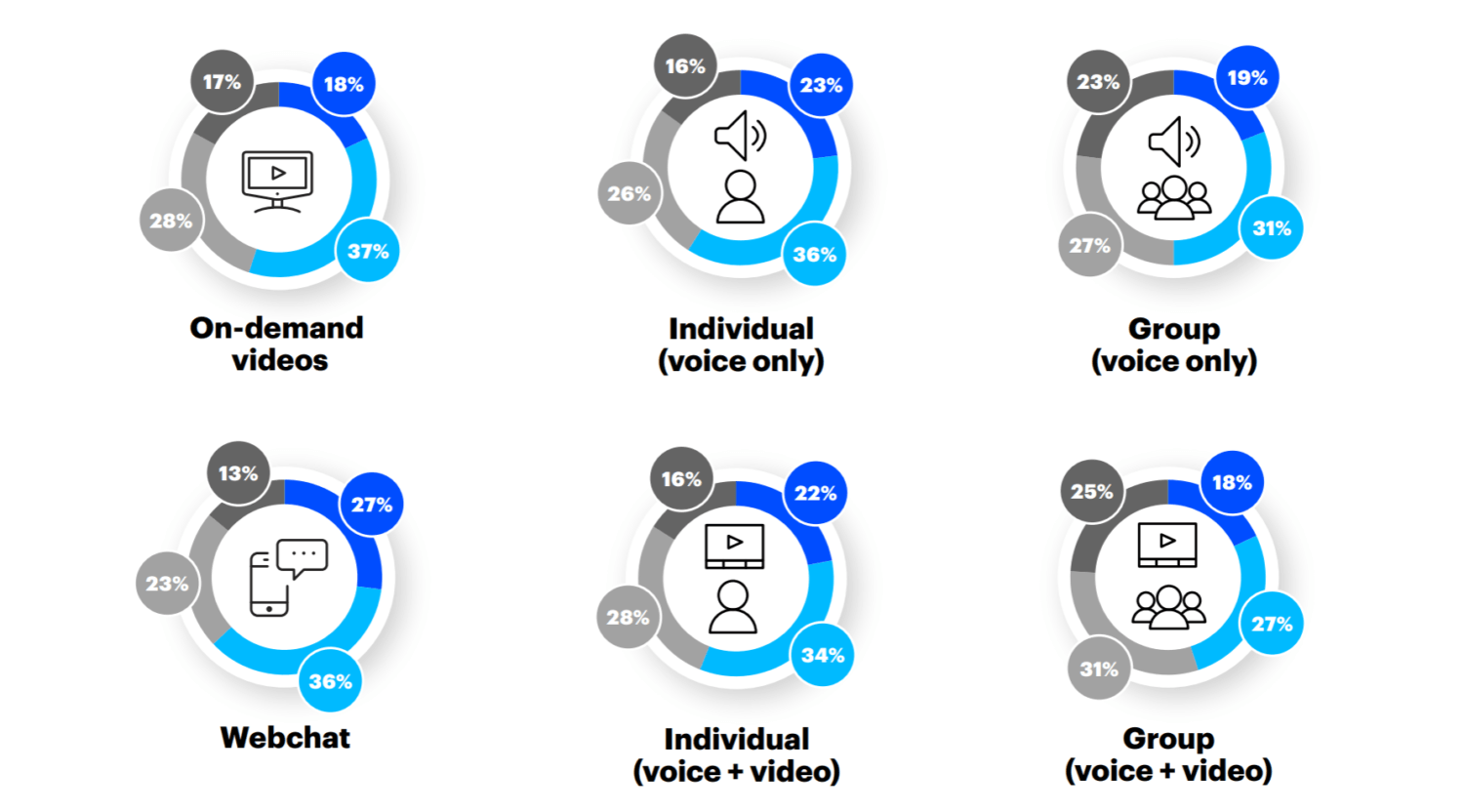
Among the channels respondents said they’d be willing to use include on-demand
videos (cited by 55%), webchat (63%), individual therapy via voice (59%) and
individual therapy via voice plus video (56%).
The research shows younger patients are much more likely than older ones to engage in virtual behavioral health services. The report notes that this is critical insight for employers as they develop their workforce and talent strategies, particularly since millennials comprise the largest percentage of the U.S. labor force, followed by Gen Zers.
In addition to improving people’s lives, better access to care and treatment is a potential breakthrough in terms of overall outcomes and medical spending as behavioral health patients typically have co-occurring medical conditions and as a result, can have two to three times the amount of associated health expenditures. Related Accenture analysis shows that even a 1% increase in treatment for behavioral health disorders in the U.S. could yield as much as $2.4 billion in medical cost savings annually, due largely to the fact that individuals with behavioral health conditions often have other medical conditions.
From Tipping Point to Transformation
The report notes three fundamental factors that healthcare providers should consider to remain relevant and responsive to consumers’ needs:
· Control the personal cost. Four in 10 respondents (44%) said they would only use such channels if the services are provided at low or no cost to them. Public and private organizations sponsoring these solutions will need to think through how to lower costs to consumers—particularly those in need.
· Orbit around experience. Beyond cost, consumers want convenience and positive user experience. While consumers are hungry for behavioral health services through virtual channels, the design of the programs and consumers’ experiences will make or break adoption no matter the demand.
· Make all the connections. Coordination and integration of care with a whole-person approach is critical. Services should be offered in the context of individuals’ physical health, and data-sharing and interoperability among different healthcare stakeholders are critical to providing the most effective care.
Report Background/Methodology
For the Accenture 2020 Behavioral Health Consumer Survey, Accenture surveyed 3,448 US consumers ages 13 and over to better understand attitudes and behaviors related to virtual health options for treating mental health conditions and substance abuse issues. All survey respondents were either diagnosed with and/or had symptoms related to specific mental health conditions such as anxiety, depression, PTSD, ADD/ADHD, or reported themselves as having addiction issues. Survey respondents received anonymity and represented a cross-section of the population based on age, location, ethnicity, insurance coverage, gender and income. The survey was conducted by Dynata in May and June 2020.
