Editor's Note: David Dyke is the Vice President of Product Management & Business Development at RelayHealth where he is responsible for delivering innovation and value to the healthcare providers across revenue cycle management. Among the processes that influence the healthcare revenue cycle, pre-authorization stands out—but not in a good way. It lacks the foundation of a widely-adopted electronic data exchange, resulting in repeated manual, ad hoc methods of securing and confirming payer
Read More
Relay Health
RelayHealth Financial’s New Tool Takes the Mystery Out of EDI Claims Status Responses
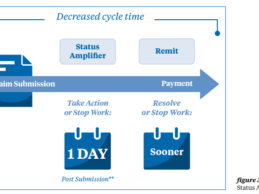
RelayHealth Financial has introduced RelayAssurance™ Status Amplifier, a new software service that automatically tracks down, inspects, and reports accurate reasons for non-payment on claims. Receiving a 277 response means there’s an update on a claim but to find out what changed (approved? denied? payment pending???) providers have to manually go into each payer portal and dig around or call and sit on hold to find out the real status.Starting today, providers can quickly learn and act on
Read More
Report: Only 1.6% of Claims Have Been Denied Post ICD-10
Of the $810 billion in claims processed by more than 2,400 hospitals and 630,000 providers using RelayHealth Financial clearinghouse, just 1.6% have been denied. This denial rate has remained unchanged since November and represents approximately $12.9 billion in denied claims since October 1st. The disclosed denial rate data from RelayHealth Financial is based on for more than 262 million claims processed between October 1, 2015 and February 15, 2016. A low denial rate indicates a healthy cash
Read More