Many Medicare Advantage health plans (35%) struggle with internal challenges in keeping pace with growth, including technology and infrastructure limitations, according to results of its latest Voice of the Market Survey. In addition, 33.8% struggle with a lack of IT staff or resources to make necessary changes and 29.4% lack the in-house Medicare experts necessary to implement adjustments in response to business fluctuation.
The survey was commissioned by HealthEdge and conducted by Survata, an independent research firm in San Francisco. Survata interviewed 201 online respondents between June 5, 2019, and June 17, 2019.
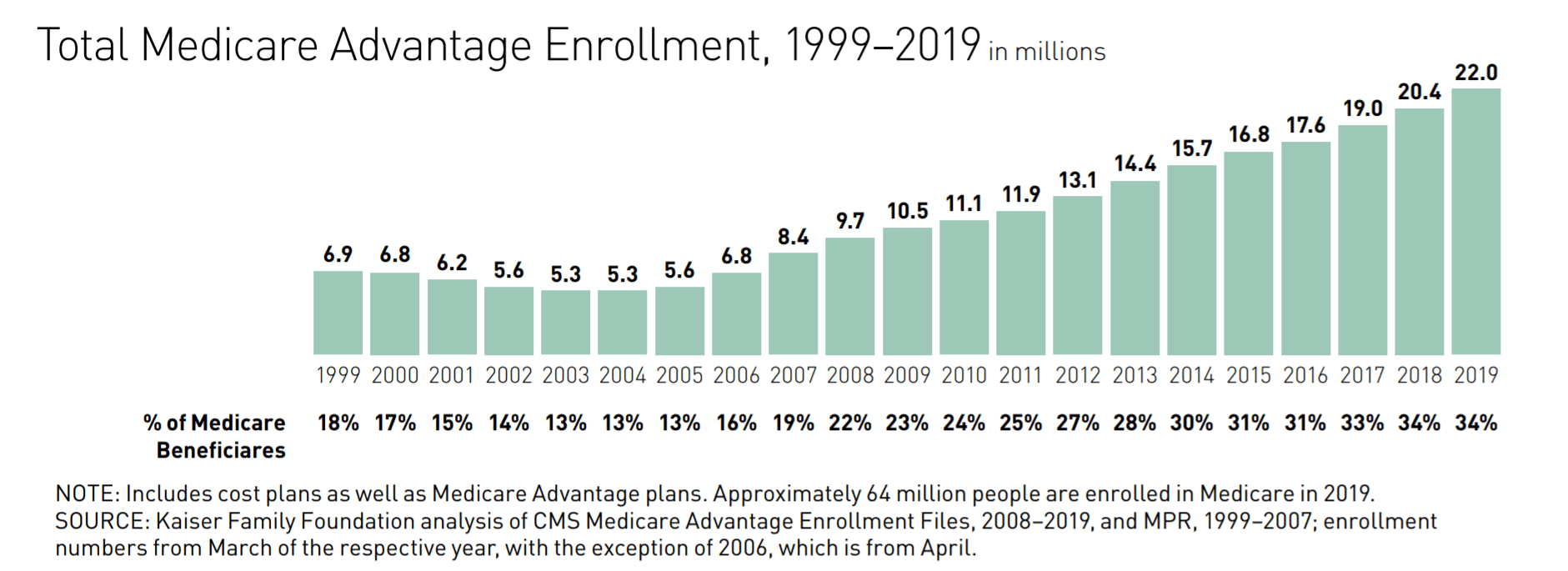
Growth of Medicare Advantage
More than 11,000 baby boomers turn 65 each day and enter the Medicare market. While sales and marketing to this population are important for growth, the survey found insurers are focused on other ways to grow their Medicare Advantage business. Medicare Advantage offerings have exploded in the last few years. After remaining flat for four years, the total number of Medicare Advantage plans increased 34 percent in the last two years to 2,734. The increased number of plans has expanded options for enrollees and created competition amongst insurers. The average recipient is able to choose between 24 plans in 2019, compared to 19 two years earlier.
The survey, designed to understand how payers are addressing the influx of the increasingly demanding and tech-savvy baby boomer population found that 92 percent of those who work exclusively in the Medicare or Medicare Advantage lines of business are currently growing, or plan to grow, their Medicare Advantage businesses at a faster rate than their traditional Medicare business.
Future Growth of Medicare Advantage Plans
The future growth of Medicare Advantage plans respondents expect to:
– Optimize value-based care programs (23.4 percent)
– Modernize technology systems to support business needs (21.4 percent)
– Invest in more people (20.9 percent)
– Design and refine high-performing networks or ACOs (18 percent)
– Ramp up sales and marketing efforts to attract new members (16.4 percent).
Attracting New Members to Medicare Advantage plans
When asked what steps organizations are taking to attract new members, respondents stated
– standard marketing and advertising to prospective members (27.4 percent)
– Social determinants of health (SDOH) (24 percent)
– incentives for healthy behavior (22.4 percent)
– appealing to tech-savvy digital consumers (14.9 percent)
– moving to new geographies (14.9 percent)
“As we move into the third decade of the 21st century, Medicare Advantage plans must keep pace with today’s seniors, who are more technologically savvy than the generation before them and who expect more from their health plans as a result,” said Steve Krupa, CEO of HealthEdge. “Our survey shows that organizations are investing more than ever in modernizing technology systems that will best position them to attract new members while continuing to meet the needs of current beneficiaries.”
