Laurie Hawkins, project manager of the Victorian Human Services Directory in Australia discusses how public health data mapping can improve global health.

HIT Consultant recently spoke with Laurie Hawkins, project manager of the Human Services Directory (HSD), about the opportunities of the National Health Service Directory (NHSD) and what can be achieved by many different stakeholders, both public and private. In our discussion, Mr. Hawkins explains why working with open health data directories and visualization of health access offers so much potential to change healthcare systems, and why its important, for both doctors and patients, to embrace the opportunity. A wider implication is that the initiatives Hawkins describes are examples of excellence in the HIT world, which provides other healthcare systems with valuable experiences and lessons learned to implement similar approaches.
Q
Can you tell us more about your background and work in healthcare technology?
I have been involved in Health Information Technology for the last twenty years, and for the past five years, project manager of the Human Services Directory, a Victorian Government e-health initiative. The HSD is a directory of Human and Health Services data, which contains service and practitioner details, contact details opening hours, location, national health identifiers for both organisations and providers, geo-coded service locations and much more. Given the success of the HSD in Victoria, it has now evolved into the National Health Services Directory (NHSD) supported by the Australian Federal Government and all Australian States and Territories. The NHSD has become a vital component of e-health infrastructure across Australia and there is now an International Standard for “Service Directories” based on the HSD.
Q
Tell us more about the National Health Service Director (NHSD), where is it applied, and how it can help patients and clinicians?
The NHSD is a national database of health and human services and represents a significant knowledge base which can be used by clinical and hospitals systems connecting to the NHSD service for functionality such as eMessaging, health planners for policy, health consumers finding health services (Doctors, Pharmacies, Emergency Departments) on their Smartphone Apps, and for organisations that provide services. Initiatives which are using The NHSD include Secure Messaging, Health portals, national health programs such as Nurse Triage, GP after Hours, Aged Care and Emergency Services.
An example of a community based initiative targeted to empowering health consumers using services data from the NHSD infrastructure is the ArthritisMap*, a tool created by a Not-for-Profit organisation, Arthritis and Osteoporosis Victoria in 2011. This initiative brings together 10’s of datasets into one website, so people with arthritis and other musculoskeletal sufferers can better self-manage their conditions by allowing them to find services and health related information on musculoskeletal disease. In the following example Doctors (Yellow), Pharmacies (Blue), Chiropractors (Orange) can be seen in the township of Bendigo on a simple to use Google Map. Detailed information such as phone numbers, opening hours, addresses found, whilst links to information brochures, camps, and other events can also be accessed.
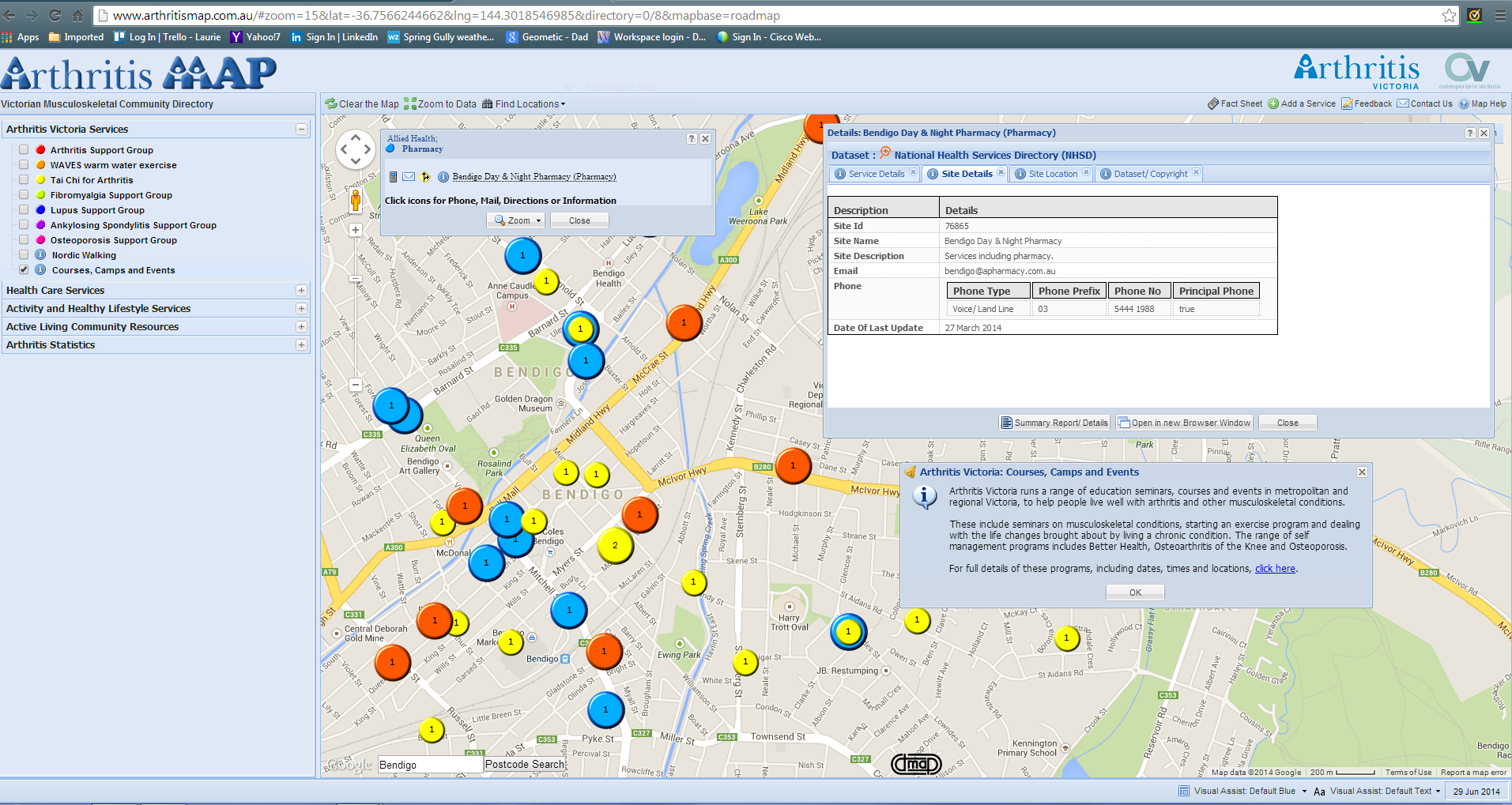
Q
What are the barriers you came across?
Barriers such as cost, technology, and data quality are common ones that have arisen. However by demonstrating what is possible with the vast knowledge of health data coming from the “Cloud”, and how effective it can be in, health planning, evidence based policy making and empowering health consumers, the barriers are more readily overcome. Data quality is improved as we can now have national data standards.
In addition, the NHSD is a shared piece of national infrastructure and allows many stakeholders to have varying degrees of control and opening up the NHSD infrastructure to be ubiquitously available, has built a community of positive support because of its utility and ease of availability. The NHSD is currently accessible via websites, mobile apps and APIs, integrated into an increasing range of software products.
Q
How important is data visualization for patients and health planning? Are there risks?
Visualization of data is extremely effective in allowing complex datasets to be brought together to convey information in a simple Geo-Spatial (Google Maps) format. A national health map is about to be released using data from the NHSD, from which we can introduce a wide range of national datasets (e.g. census) and local health datasets to support a greater focus on evidence based planning and decision making.
Following is an example of a visualization, using the ArthritisMap, the Health Planning Tool mentioned above, in which citizens from Victoria should be within 10 km of an Emergency Department (Red) in Melbourne. Planning circles have been used and combined with Urban Growth Boundaries (Yellow), and the numbers of Residential Housing Developments (Green). This demonstrates areas where communities will increase so based on this scenario, Emergency Departments still need to be built to cope with the increased population.
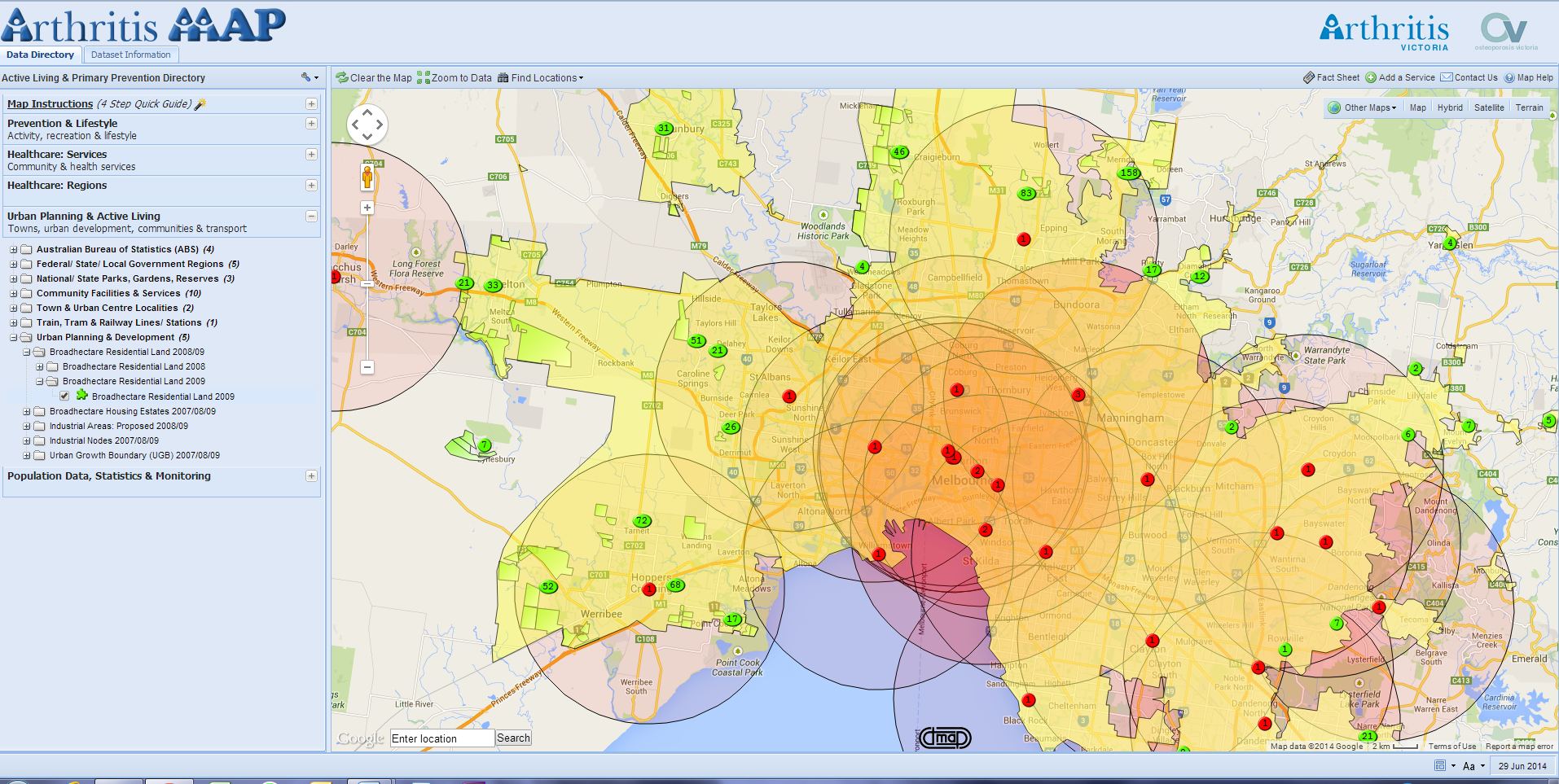
Now that key service information can be sourced (from an authoritative resource) and greater focus on data governance rather than fragmented silos, data quality issues are reduced and we are opening up more data possibilities to the greater community as it allows greater/more widespread use of data.
Q
The solutions you worked on does work for Australia. Would this approach work anywhere, to add value to healthcare communities and research?
This could be replicated anywhere around the world. For example National Human Services Directories linked together across the European Union to provide health consumers, health planners, research groups with a significant database of health and human services. This could empower citizens when they travel, they can see where Doctor (General Practitioner) services are available after hours on the user’s smartphone. Going further, integration with these NHSD’s and adoption of a Health Planning Tools would allow health planning to address increasing demands on health systems and exchange of data across borders in a secure manner, all from the Cloud.
Q
Where do you see the future for data presentation and visualization in 10 years?
As we move rapidly into a Virtual World, Open Health Data is an essential resource which will be increasingly used to address the long term health challenges. For example, Global Health Organisations can find where health services are located, the incidence of a disease and profile of the population in a particular area, then provided appropriate resourcing. These services could be found by having a Federated International Health and Human Services Directory drawn from National Health Services Directories.
With increasing demands on global health services, we urgently need to shift from Primary and Acute Care to building healthy communities through knowledge based environmental preventative strategies and sustainable active living principles. This can be done here and now by making data readily available in a more effective context to policy makers, health planners and researchers.
Just as important to addressing long term health demands is to empower citizens making data available to realize its full potential as their engagement is critical to the success of our communities to better managing their conditions, and improving health literacy.
The “NHSD” is an excellent examples of “storing data once, using many times”, the opportunities around data are endless, we just have to grasp them.
Ben Heubl is a digital health advocate, activist and journalist for health 2.0 innovation.Ben Heubl is speaker at various healthcare innovation conferences and events, a TEDMED delegate, founded the non-for-profit organization Health 2.0 Copenhagen, Mentor at the HealthXL accelerator, and currently passionately writes for various online magazines in the context of digital health innovation and technology. Ben also currently supports a UK health innovation SME to change how citizens access healthcare. You can follow him on Twitter at @benheub
