What You Should Know
- The Launch: UnitedHealthcare (UHC) has introduced Avery, a generative AI companion integrated directly into the UnitedHealthcare app and myuhc.com.
- The Scale: Avery is currently live for 6.5 million employer-sponsored members and 160,000 Medicare Advantage members. UHC plans an aggressive expansion to reach 20.5 million members across commercial, Medicare, and Medicaid plans by the end of the year.
Beyond the Chatbot: Agentic Healthcare
For years, health insurance chatbots have been little more than glorified FAQ search bars. If a member asked a question more complex than “Where is my ID card?”, the bot would typically fail, forcing the frustrated patient to call a 1-800 number, wait on hold, and explain their entire problem from scratch to a customer service agent.
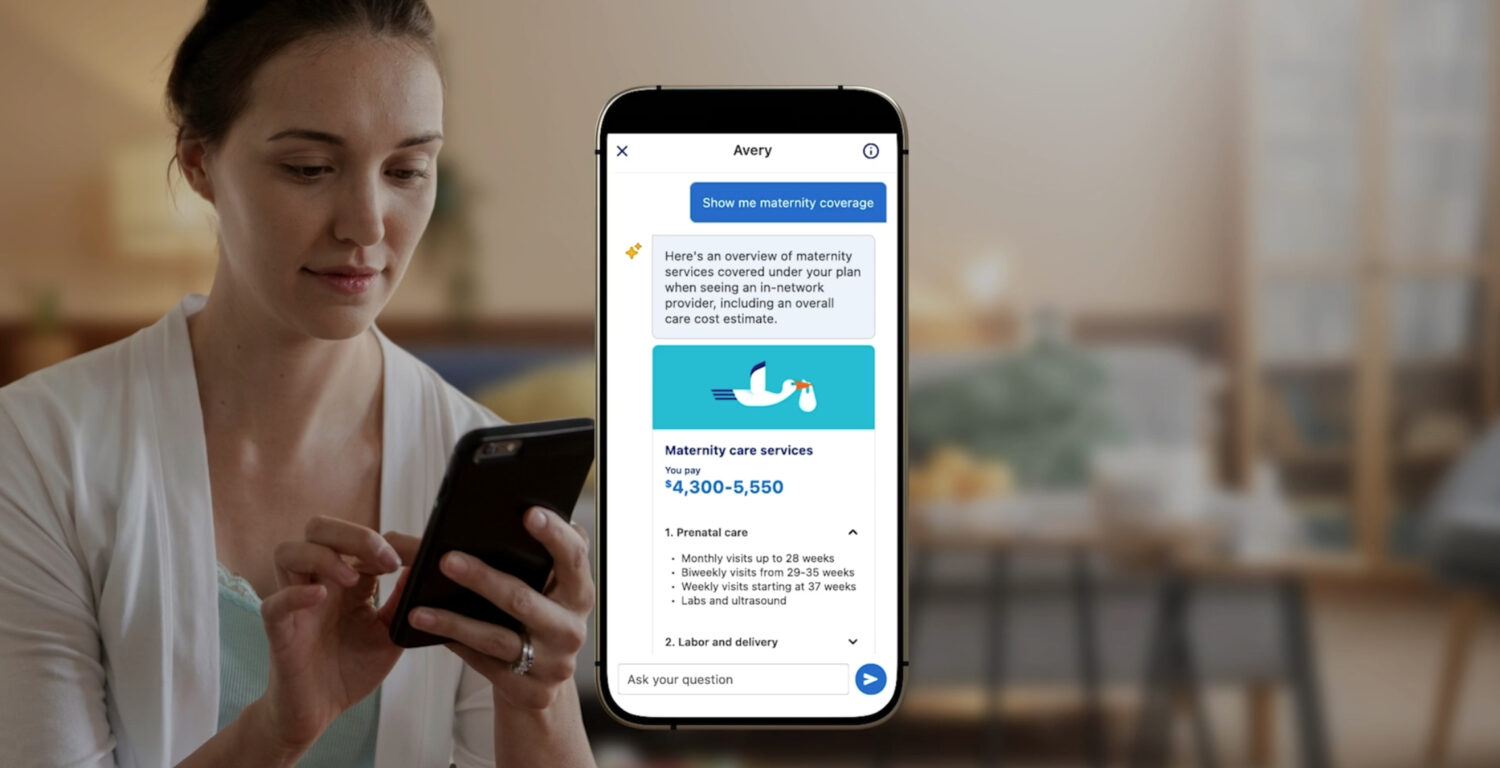
Avery doesn’t just read your benefits summary back to you. If a member needs to see a doctor, Avery can analyze their specific coverage details, compare care options based on cost, and then—crucially—actually call the network primary care provider to schedule the appointment on the member’s behalf. This transitions the AI from a passive information portal into an active care coordinator.
The operational results of this capability are staggering. UnitedHealthcare reports that 90% of the time, members who engage with Avery are able to resolve their issues without ever needing to speak to a human advocate.
“People want health care to be easier to use and tailored to their personal needs,” said Dan Kueter, CEO for UnitedHealthcare’s commercial business. “Avery is one way we are responding to consumer demand for a more coordinated and simpler experience.”
The Call Center ROI & Handoff
Currently, 90% of the time, members using Avery do not require assistance from a human advocate. When an issue is too complex for the AI, Avery automatically transfers the member to a live customer advocate. But instead of the advocate starting blind, Avery instantly generates a full synopsis of the member’s history, intent, and uploaded documents. The advocate spends less time taking notes and digging through databases, and the member is spared the infuriating task of repeating their problem.
Parent company UnitedHealth Group is investing $1.6 billion into AI this year.
