Dr. Donald Voltz, MD discusses how the electronic medical records of today is merely a duplication of the past and how future EMR systems must align medical professionals with data that needs to be collaborative.

The open question regarding Electronic Medical Records (EMRs) is what they now offer the medical community and what would medical professionals need and envision for the next generation.
The Henry Ford adage: “If I had asked people what they wanted, they would have said faster horses.” This quote has been used to counter criticism from physicians with respect to EMR adoption and use. This would be a more solid argument if EMR’s brought novel and impactful power to the delivery of healthcare, but today’s EMRs are nothing more than the electronic duplication of the medical record that has existed since the 20’s.
Errors and Duct Tape Solutions
Having personally used the three largest EMR’s, I am amazed at the errors present in the systems and the use of duct tape solutions such as scanning paper records into the system rather than integration with other healthcare systems. The most widely deployed hospital EMRs are built upon database technology from the 60’s. The user experience, with patient data entry and the access of that data for care management are rudimentary at best.
With these systems costing hospitals millions of dollars, expectations should be greater. The cost of replacing current EMRs when other advancements arrive is one possible solution, but this is not likely for hospitals due to the costs involved. Looking for solutions that can offer a collaborative way to connect all of the proprietary data models while focusing on interfaces that enhance patient and physician usability seem to be a better solution.
Physicians, patients and the healthcare industry should expect EMRs to at least support physicians and other healthcare providers in accomplishing their goal of taking care of patients. Unfortunately, many social media platforms sport far more usability and access to information than EMRs, while maintaining security and integrity of data.
Many new technologies will be developed and applied to these systems, but we need to have a better solution than proprietary companies completing all of the EMR development. EMR vendors need to integrate around collaborative connectivity hubs like the nurses sheet many of us used. Too much is at stake for hospitals to maintain all these legacy systems; we must as an industry look for new ideas. Sure, there are work arounds being employed to address the deficiencies in these systems, but most are not ideal and result in higher costs to systems that were touted to reduce the delivery of care.
Related: Can EHRs Achieve the Interoperability We Need?
Medical Scribes Are Not the Answer
The most concerning issue to me with respect to EMR productivity is the use of medical scribes. There is no question that the use of these systems and the requirements for entering large amounts of patient information by physicians decreases their productivity and reduces direct patient contact time. There is no practical way to reduce the amount of patient information, so physicians employ medical scribes to enter data which opens up more time for patients.
This trend will increase the cost of healthcare and reduce the original premise that EMR’s would increase physician efficiency. A better designed system would enable a practitioner to customize their documentation to the workflow they have found most effective and efficient for them.
Coping with EMR Scavenger Hunt
An ability to connect with a single interface, irrespective of the EMR, would improve my day-to-day patient care and create standardization for where EMR information is stored. Currently, I have to look in multiple places within EMR’s to gather all of the relevant pieces of information to manage a patient’s complaint or condition. This reminds me of a scavenger hunt and not the well designed dashboard that was promised.
Instead of identifying the problems of paper-based medical charts and developing tools to overcome their limitations, we added technology to the same paradigms. This only resulted in improved readability, but not an improvement in how physicians access the information of these systems.
Switching between different locations to gather vital sign information, review past medical history, and laboratory studies is not only manual, but data can be entered in different ways, depending on the healthcare provider who entered the information in the system. Switching between views, use of a non-standard interface and the use of scribes to enter information will continue to prevent the real advances EMR technology needs.
Related: Why Physicians Will Never Ever Like EMRs and How to Change That
Lack of Communication
The medical record is a log of patient data, the thoughts of physicians and other healthcare practitioners, and a log of the care delivered. It is above all, a means of communicating with one another. The EMR, being closely modeled to the standard paper-based medical record, serves these purposes with the promise of improving oversight and error detection. The potential reach of the medical record extends far beyond that of it paper predecessor and once the issues with interoperability have been addressed, more value will be added. However, its use as a communication tool does not yet extend beyond paper. Although remote access capabilities exist, these do not make it an enhanced communication tool.
A user of the medical record still has to search through the information it contains. When a piece of information is not present, the user has no way of knowing if it is not yet done, an order missed, the data never entered, or it was entered into a non-standard area of the medical record.
These issues can cause duplication and medical errors when information is not acted upon. Most everything done in healthcare carries required action behind it, be it the request for specialized consultation, the ordering of labs or tests, or the interpretation of nursing notes and vital signs. It is often not clear from EMR’s when a piece of information has been assessed and possibly acted upon.
Related: What is the Future Role of EHRs in the Health IT Ecosystem?
“Smart” Hub Collaborative Data Needed
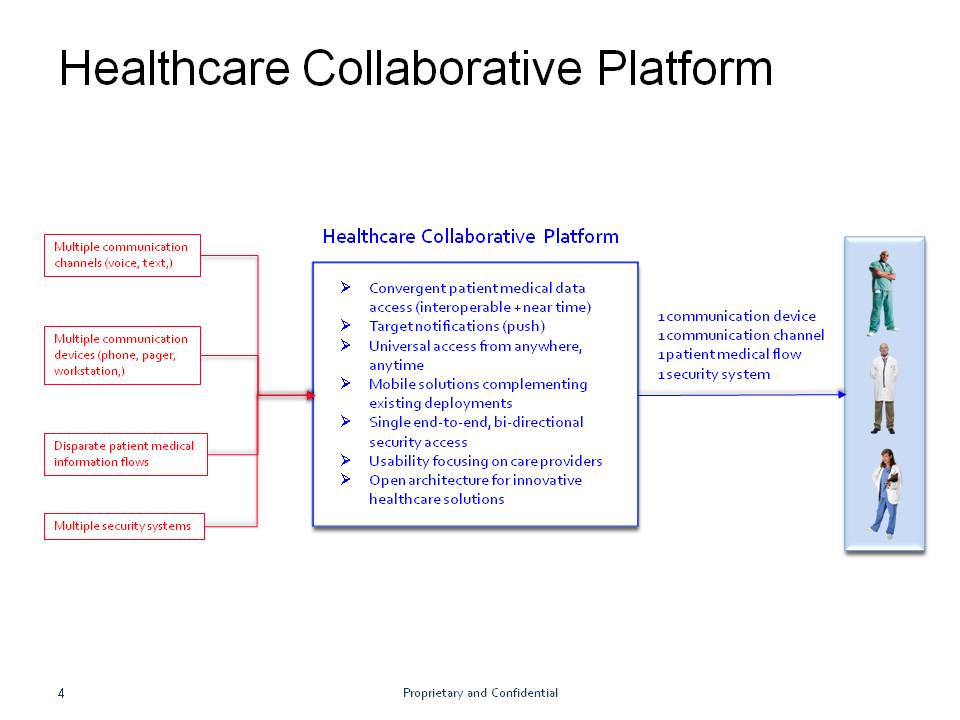
We need a system to align medical professionals with data that needs to be collaborative, not passive, and include analysis with the right data delivered to those who need it, when they need it, with all the data in one place. Systems that make the data “smart” through collaborative platforms that can analyze and interpret the data.
What I find frustrating is that this technology exists to make EMR’s a communication platform that can embrace standard technologies that have been validated in other areas such as finance that push information out to physicians and others who are caring for patients. Reversing the need to search for necessary information and replacing it with push technology would make EMR’s more useful and efficient for everyone.
I do not expect perfection on the first iteration, but I would like to see early adaptors be able to add customization or develop tools that could enhance these systems. Those of us working in the trenches to enhance our patient’s experience from a safety and quality standpoint need the ability to develop on top of existing systems. There are many innovative physicians I know who could bring change if tools and interfaces into EMR’s were available.
I fully understand the issues with securing and protecting patient information. We have developed a lot of experience with respect to accessing and sharing information between systems. Standardized protocols exist for transmission of information as well as systems to evaluate and certify technology prior to release into clinical care.
Imagine what a platform such as Apple’s App Store would have in the area of EMR’s? Harnessing the frustration of physicians eager to learn about and develop tools to enhance EMR’s would expand functionality. Granted there would be many less than novel applications developed, but there would also be some blockbusters that would revolutionize electronic documentation. Healthcare, like every other business sector, has a subgroup of innovative explorers who embrace the current frustrations and barriers to find ways to overcome them. I am just one.
Related: Looking Beyond the EHR: Know Your Data, Control Your Story
Written by Dr. Donald Voltz,MD, Aultman Hospital, Department of Anesthesiology, Medical Director of the Main Operating Room, Assistant Professor of Anesthesiology, Case Western Reserve University and Northeast Ohio Medical University. Thanh Tran, CEO of Zoeticx, Inc. also contributed.
Dr. Voltz is a board-certified anesthesiologist, researcher, medical educator, and entrepreneur. With more than 15 years of experience in healthcare, Dr. Voltz has been involved with many facets of medicine. He has performed basic science and clinical research and has experience in the translation of ideas into viable medical systems and devices.
photo credit: Yann Ropars via cc